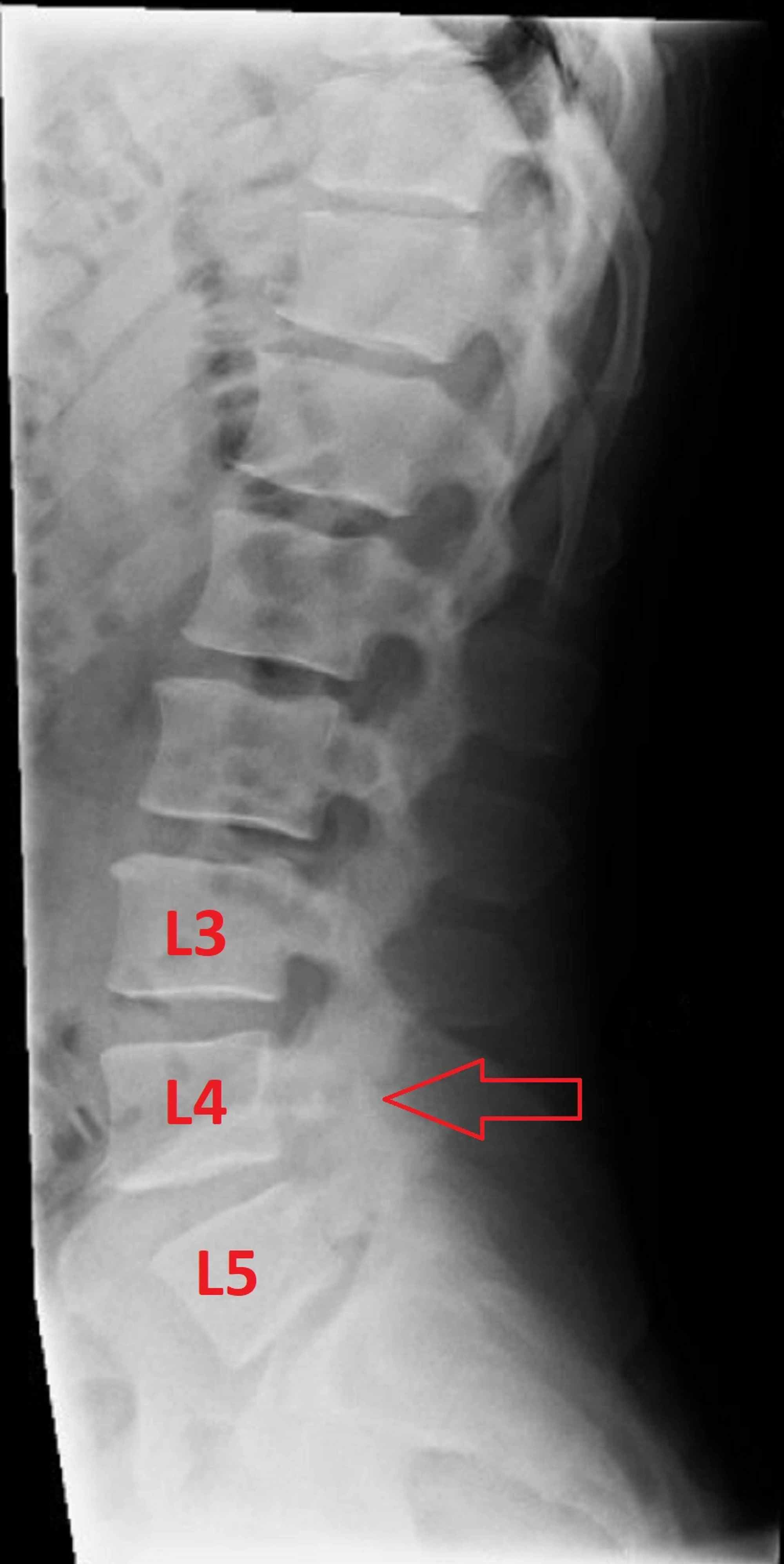
In fact, these intrasegmental fixation techniques abovementioned cannot be stronger than intersegmental pedicle screws in the control of low lumbar extension and rotation stress. Pedicle screw-hook or U rod methods are able to provide more stability however, the L5 lamina often has developmental abnormalities which make the pedicle screw and hook too close to have enough room for tightening the link to compress the bone graft in the defect. 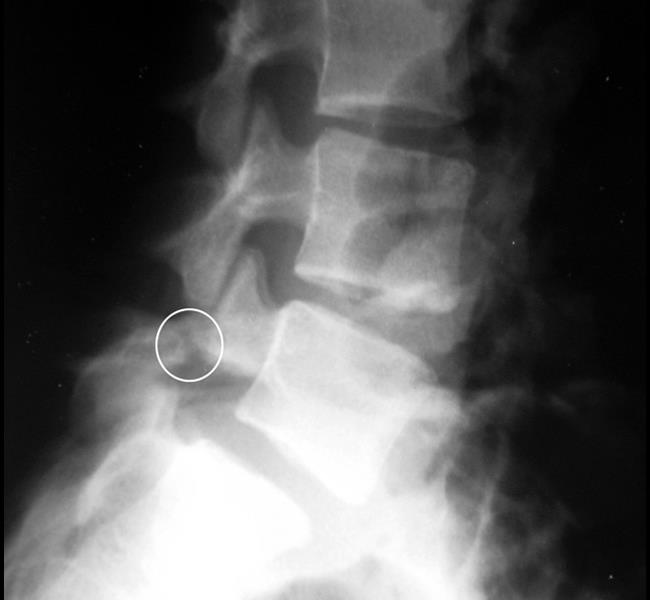
Wiring techniques have the disadvantages of more bleeding, wire break, and insufficient stabilization. Furthermore, the screw occupies the bone graft area for fusion. Implanting a screw across the par is technically difficult with high incidence of screw fracture. A number of techniques had been described for repair by intrasegmental fixation with good results. The points of surgery are pars defect debridement, bone graft, and local stabilization. The concept of repair surgery is similar to osteosynthesis. Meaningless sacrifice of fairly normal disc and segmental motion make stricter indication for fusion. Surgical methods for lumbar spondylolysis could be roughly divided into two categories, fusion and repair. The aims of surgery are to reduce pain, stabilize affected segment, promote healing of pars defect, and control spondylolisthesis development effectively. When they fail to respond to conservative treatment, surgical interventions may be required. Symptomatic spondylolysis should be first treated by nonoperative care, despite several operative options available. A study in Japan described 70% of patients with bilateral pars defects are associated with varying degrees of vertebral spondylolisthesis, and some cases need surgery. One fourth of individuals with spondylolysis may suffer from LBP. 
The condition is often asymptomatic but may be the cause of low back pain (LBP) in young adults. Most of spondylolysis are found at L5 level. Previous studies showed repetitive lumbar extension and rotation were related to the development of spondylolysis. The current theory believes fatigue or stress fracture of pars with developmental factors is the most widely accepted reason for the occurrence of isthmic defect. Lumbar spondylolysis is a bony defect in the pars interarticularis. This technique is reliable for spondylolysis repair which has satisfactory symptom relief, high healing rate, low incidence of complications, and preserve a large part of ROM for fixed segment. ConclusionsĪlthough sacrificing L5S1 segment motion temporarily, more stability was obtained with intersegmental fixation. There were 3 patients of delayed incision healing without other complications. The rates of L5S1 ROM preservation were 79.8% and 64.0% after fixation removal at 1 and 2 years postoperatively. JOA score increased significantly postoperatively (P < 0.05) with average improvement rate of 79.3%. Low back pain VAS significantly (P < 0.05) improved from preoperative mean value of 7.2 to 1.3 at the final follow-up postoperatively (P < 0.05). The union rate of pars was 82.0% at 12 months and 94.3% at 24 months postoperatively. There were 97 patients (194 pars) followed with mean follow-up of 23 months (range, 12–36 months). After fixation removal, the rate of ROM preservation at L5S1 was calculated. The healing time, complications, number of spina bifida occulta, Japanese Orthopedic Association (JOA) score, and VAS for back pain were recorded. The sagittal and axial CT images were used to determine the bone union. The diagnostic block test of L5 bilateral pars defect was done in all patients preoperatively. According to CT scan, the spondylolysis were classified into 3 categories: line, intermediate, and sclerosis type. MethodsĪ retrospective analysis of 128 patients with L5 spondylolysis treated with this method was performed. The aim of present study is to assess the clinical outcomes of L5 symptomatic spondylolysis with this technique. We reported a repair technique with temporary intersegmental pedicle screw fixation and autogenous iliac crest graft. A number of techniques have been described for repair by intrasegmental fixation with good results however, there are still some problems. When symptomatic spondylolysis fail to respond to nonoperative treatment, surgical management may be required.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
